Claims qualification criteria are the specific rules a claim must satisfy before an insurer agrees that the loss is eligible for review, payment, or benefits.
It is not about pricing.
It is not about coverage limits.
It is about whether a claim is allowed to enter the system at all.
For high-risk workers, many claims fail before they are ever evaluated.
What Claims Qualification Criteria Mean
Before an insurer considers paying a claim, it checks whether the claim qualifies.
Typical qualification criteria include:
-
Whether the injury is work-related
-
Whether the incident falls within covered activities
-
Whether reporting timelines were met
-
Whether documentation is complete
-
Whether exclusions apply
If any required criterion fails, the claim may be rejected without further review.
These criteria operate alongside coverage activation thresholds, determining whether a claim is even allowed to enter the review process.
What Breaks When a Claim Fails Qualification
When a claim fails qualification criteria:
-
No claim file is formally opened
-
No coverage analysis is performed
-
No medical causation review occurs
-
No benefit calculation is triggered
-
Appeals are limited to procedural correction, not claim merits
The claim does not move deeper into the claims system.
It effectively never exists for evaluation purposes.
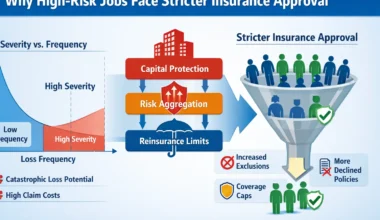
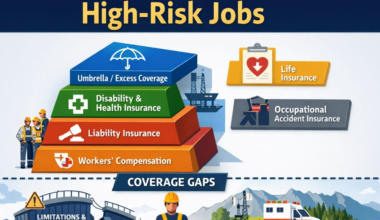
Why High-Risk Insurance Uses Strict Qualification Rules
High-risk insurance faces:
-
High claim frequency
-
Large potential losses
-
Greater fraud and dispute risk
To control exposure, insurers enforce strict front-end filters.
Qualification criteria act as a gatekeeping mechanism, reducing how many claims proceed deeper into the system.
Insurance regulators such as the National Association of Insurance Commissioners describe how insurers apply eligibility and reporting rules before claims are reviewed.
How This Affects Workers
Claims qualification criteria mean:
-
Claims can fail early and silently
-
Denials may occur without medical review
-
Technical errors outweigh injury severity
Workers often believe denial means disbelief.
In reality, it often means failure to qualify.
Why Qualification Is Often Confused with Denial
Insurers rarely explain the distinction.
Qualification rules are embedded in:
-
Definitions
-
Reporting clauses
-
Procedural conditions
Workers experience qualification failure as denial, even though evaluation never occurred.
When claims fail qualification, the result often appears identical to claims denial, even though no substantive evaluation occurred.
In the Risk Job Insurance System
Claims qualification criteria explain why:
-
Claims are rejected immediately
-
Appeals fail early
-
Coverage feels conditional even after activation
They are the first barrier a claim must cross to exist.
This definition forms part of the broader Risk Job Insurance framework, which explains how high-risk coverage systems are structured, enforced, and administered across occupations.
This entry is part of the Risk Job Insurance Definitions hub, which organizes and explains the core systems, terms, and mechanisms that govern high-risk insurance coverage.